SKYSONA is the first FDA approved therapy shown
to slow the progression of neurologic dysfunction in boys with this
devastating and fatal neurodegenerative disease
Management team to host conference call Monday,
September 19, at 8:00 a.m. ET
bluebird bio, Inc. (Nasdaq: BLUE) today announced the U.S. Food
and Drug Administration (FDA) has granted Accelerated Approval of
SKYSONA® (elivaldogene autotemcel), also known as eli-cel, to slow
the progression of neurologic dysfunction in boys 4-17 years of age
with early, active cerebral adrenoleukodystrophy (CALD). The
Company also confirmed that the previous clinical hold on the
eli-cel clinical development program has been lifted.
CALD is a rare, progressive, neurodegenerative disease that
primarily affects young boys and causes irreversible, devastating
neurologic decline, including major functional disabilities such as
loss of communication, cortical blindness, requirement for tube
feeding, total incontinence, wheelchair dependence, or complete
loss of voluntary movement. Nearly half of patients who do not
receive treatment die within five years of symptom onset. Prior to
the approval of SKYSONA treatment, effective options were limited
to allogeneic hematopoietic stem cell transplant (allo-HSCT), which
is associated with the risk of serious potential complications
including death, that can increase dramatically in patients without
a human leukocyte antigen (HLA) matched donor.
“Children with CALD and their families have been at the heart of
bluebird’s mission since the company was founded more than a decade
ago,” said Andrew Obenshain, chief executive officer, bluebird bio.
“For the ALD community, this long-awaited approval represents
significant hope and offers families a new option where, for many,
there had been none. We are grateful to every individual who was
involved in the development of SKYSONA and are committed to working
with providers and payers to make this important treatment option
available to patients and their families.”
“The agony of watching your child slip away is something no
parent should have to bear,” said Elisa Seeger, co-founder, ALD
Alliance. “We have made significant strides in providing children
diagnosed with CALD the best chance at life with early
identification of ALD through expanded newborn screening. Yet with
limited treatment options, early diagnosis is still cause for
despair instead of hope for many families. Today, parents whose
boys receive a CALD diagnosis can have renewed hope for the
future.”
“CALD strikes young boys in the prime of their development,
robbing them of core neurologic functions necessary for survival.
That is an unimaginable reality for any parent, and as a clinician,
it is heartbreaking to have limited treatment options for these
children and their families,” said David A. Williams, MD, Chief,
Division of Hematology/Oncology, Boston Children’s Hospitali.
“After supporting the clinical development of SKYSONA for nearly a
decade as a study site, Boston Children’s Hospital is extremely
pleased that an FDA-approved therapy is now available for children
who urgently need new therapies.”
“As one of the largest and most experienced pediatric gene
therapy and stem cell transplant programs in the world, the
University of Minnesota is committed to expanding access and
advancing care and research for patients with rare diseases like
ALD,” said Paul Orchard, MD, a pediatric blood and marrow
transplant physician at the University of Minnesota Medical School
and M Health Fairview Masonic Children’s Hospital. “It’s crucial
for these patients and families to have another therapeutic option
for cerebral ALD beyond blood stem cell transplantation utilizing
cells from another donor, and we’ve seen firsthand the impact that
gene therapy has on our patients. We are encouraged by progress
we’re making to treat these rare and devastating diseases.”
As a condition of the SKYSONA Accelerated Approval, bluebird has
agreed to provide confirmatory long-term clinical data to the FDA.
bluebird anticipates that this will include data from the ongoing
long-term follow-up study (LTF-304), which follows patients treated
in clinical trials for 15 years, and from commercially treated
patients.
bluebird anticipates that commercial product will be available
by the end of 2022 through a limited number of Qualified Treatment
Centers (QTCs) in the United States, including Boston Children’s
Hospital and Children’s Hospital of Philadelphia.
bluebird has set the wholesale acquisition cost of SKYSONA in
the U.S. at $3.0M. Additional information is available through
bluebird’s patient support program, my bluebird support, which will
provide personalized support for patients and their families
related to all aspects of the gene therapy journey. Caregivers of
patients with CALD can visit mybluebirdsupport.com or call
833-888-NEST (833-888-6378) Monday-Friday between 8 a.m. and 8 p.m.
ET to ask questions and enroll.
The SKYSONA Biologics License Application (BLA) was reviewed by
the U.S. FDA under Priority Review, and bluebird received a rare
pediatric priority review voucher upon approval. SKYSONA was
previously granted Orphan Drug designation, Rare Pediatric Disease
designation, and Breakthrough Therapy designation.
SKYSONA Clinical Data
The approval of SKYSONA is based on data from bluebird bio’s
Phase 2/3 study ALD-102 (Starbeam) (N=32) and Phase 3 ALD-104
(N=35) study.
Both open-label, single-arm studies enrolled patients with
early, active CALD who had elevated very long chain fatty acid
(VLCFA) values, a Loes score between 0.5 and 9 (inclusive), and
gadolinium enhancement on magnetic resonance imaging (MRI) of
demyelinating lesions. Additionally, patients were required to have
a neurologic function score (NFS) of ≤ 1, indicating limited
changes in neurologic function. The efficacy of SKYSONA was
compared to a natural history population.
Per protocol, patients treated with SKYSONA were assessed using
the NFS and monitored for the emergence of six Major Functional
Disabilities (MFDs) associated with CALD progression including loss
of communication, cortical blindness, requirement for tube feeding,
total incontinence, wheelchair dependence, or complete loss of
voluntary movement.
The Accelerated Approval of SKYSONA is based on 24-month
MFD-free survival. A post-hoc enrichment analysis in symptomatic
patients assessed MFD-free survival from onset of symptoms (NFS ≥
1) in SKYSONA treated (N=11) and untreated patients (N=7). SKYSONA
treated patients had an estimated 72 percent likelihood of MFD-free
survival at 24 months from time of first NFS ≥ 1, compared to
untreated patients who had only an estimated 43 percent likelihood
of MFD-free survival.
The most common non-laboratory adverse reactions (incidence ≥
20%) are mucositis, nausea, vomiting, febrile neutropenia,
alopecia, decreased appetite, abdominal pain, constipation,
pyrexia, diarrhea, headache, and rash. The most common Grade 3 or 4
laboratory abnormalities (≥40%) include leukopenia, lymphopenia,
thrombocytopenia, neutropenia, anemia, and hypokalemia. Please see
SKYSONA Important Safety Information below, including a Boxed
Warning for Hematologic Malignancy.
Enrollment is complete and all patients have been treated in
both studies; follow-up in ALD-104 is ongoing. All patients who
complete 24 months of follow-up in studies ALD-102 or ALD-104 are
encouraged to participate in a long-term follow-up study (LTF-304)
to continue monitoring safety and efficacy outcomes in boys treated
with SKYSONA through 15 years post-treatment. On September 15,
2022, the FDA lifted the clinical hold that was put in place August
2021, prior to the completion of its review of the SKYSONA
Biologics License Application.
About Cerebral Adrenoleukodystrophy (CALD)
CALD is a progressive and irreversible neurodegenerative disease
that primarily affects young boys. The disorder is caused by
mutations in the ABCD1 gene that affect the production of
adrenoleukodystrophy protein (ALDP) and subsequently leads to
accumulation of very long-chain fatty acids (VLCFAs), primarily in
the white matter of the brain and spinal cord. This accumulation
leads to the breakdown of myelin, the protective sheath that nerve
cells need to function effectively, especially for thinking and
muscle control. The onset of symptoms of CALD typically occurs in
childhood (median age 7). Early diagnosis and treatment of CALD is
essential, as nearly half of patients who do not receive treatment
die within five years of symptom onset.
Indication
SKYSONA is indicated to slow the progression of neurologic
dysfunction in boys 4-17 years of age with early, active cerebral
adrenoleukodystrophy (CALD). Early, active cerebral
adrenoleukodystrophy refers to asymptomatic or mildly symptomatic
(neurologic function score, NFS ≤ 1) boys who have gadolinium
enhancement on brain magnetic resonance imaging (MRI) and Loes
scores of 0.5-9.
This indication is approved under accelerated approval based on
24-month Major Functional Disability (MFD)- free survival.
Continued approval for this indication may be contingent upon
verification and description of clinical benefit in a confirmatory
trial(s).
Limitations of Use
SKYSONA does not prevent the development of or treat adrenal
insufficiency due to adrenoleukodystrophy.
An immune response to SKYSONA may limit the persistence of
descendent cells of SKYSONA, causing rapid loss of efficacy of
SKYSONA in patients with full deletions of the human adenosine
triphosphate binding cassette, sub family D, member 1 (ABCD1)
transgene.
SKYSONA has not been studied in patients with CALD secondary to
head trauma.
Given the risk of hematologic malignancy with SKYSONA, and
unclear long-term durability of SKYSONA and human
adrenoleukodystrophy protein (ALDP) expression, careful
consideration should be given to the appropriateness and timing of
treatment for each boy, especially for boys with isolated pyramidal
tract disease based on available treatment options since their
clinical symptoms do not usually occur until adulthood.
Important Safety Information
BOXED WARNING: HEMATOLOGIC MALIGNANCY
Hematologic malignancy, including life-threatening cases of
myelodysplastic syndrome, has occurred in patients treated with
SKYSONA. Patients have been diagnosed between 14 months and 7.5
years after SKYSONA administration, and the cancers appear to be
the result of the SKYSONA lentiviral vector, Lenti-D, integration
in proto-oncogenes. Monitor patients closely for evidence of
malignancy through complete blood counts at least every 6 months
and through assessments for evidence for clonal expansion or
predominance at least twice in the first year and annually
thereafter; consider bone marrow evaluations as clinically
indicated.
Hematologic Malignancy
Myelodysplastic syndrome (MDS), a hematologic malignancy, has
developed in patients treated with SKYSONA in clinical studies. At
the time of initial product approval, MDS had been diagnosed in
three patients after administration of SKYSONA. The clinical
presentation for the three patients varied. Two patients who were
diagnosed at 14 months and 2 years after treatment with SKYSONA had
preceding delayed platelet engraftment. The third patient had
normal blood counts from 18 months to 5 years following treatment
with SKYSONA and presented 7.5 years after SKYSONA administration
with symptomatic anemia and thrombocytopenia and was subsequently
diagnosed with MDS with increased blasts. All 3 patients underwent
allogeneic hematopoietic stem cell transplant; 1 patient required
pre-transplant chemotherapy and total body irradiation as treatment
for excess blasts prior to transplant and 1 patient underwent total
body irradiation as part of his conditioning regimen.
SKYSONA Lenti-D lentiviral vector integration into
proto-oncogenes appears to have mediated the three cases of
hematologic malignancy. The hematologic malignancies diagnosed at
14 months and 2 years involved integration into the MECOM
proto-oncogene and increased expression of the oncoprotein EVI1.
All patients treated with SKYSONA in clinical studies have
integrations into MECOM; it is unknown which integrations into
MECOM or other proto-oncogenes are likely to lead to
malignancy.
Because of the risk of hematologic malignancy, carefully
consider alternative therapies prior to the decision to treat a
child with SKYSONA. Consider consultation with hematology experts
prior to SKYSONA treatment to inform benefit-risk treatment
decision and to ensure adequate monitoring for hematologic
malignancy. Consider performing the following baseline hematologic
assessments: complete blood count with differential,
hematopathology review of peripheral blood smear, and bone marrow
biopsy (core and aspirate) with flow cytometry, conventional
karyotyping, and next generation sequencing (NGS) with a molecular
panel appropriate for age and including coverage for gene mutations
expected in myeloid and lymphoid malignancies; and testing for
germline mutations that are associated with hematologic
malignancy.
Early diagnosis of hematologic malignancy can be critically
important, therefore, monitor patients treated with SKYSONA
lifelong for hematologic malignancy. For the first fifteen years
after treatment with SKYSONA, monitor via complete blood count
(with differential) at least twice per year and via integration
site analysis or other testing for evidence of clonal expansion and
predominance at least twice in the first year and then annually.
Consider appropriate expert consultation and additional testing
such as more frequent complete blood count (with differential) and
integration site analysis, bone marrow studies, and gene expression
studies in the following settings after treatment with SKYSONA:
- Delayed or failed engraftment of platelets or other cell lines
(patients who do not achieve unsupported platelet counts of ≥ 20 ×
109/L on or after Day 60 appear to be at particularly high risk for
developing malignancy); or
- New or prolonged cytopenias; or,
- Presence of clonal expansion or predominance (e.g., increasing
relative frequency of an integration site, especially if ≥ 10% and
present in MECOM or another proto-oncogene known to be involved in
hematologic malignancy).
If hematologic malignancy is detected in a patient who received
SKYSONA, contact bluebird bio at 1 833 999 6378 for reporting and
to obtain instructions on collection of samples for further
testing.
Serious Infections
Severe infections, including life-threatening or fatal
infections, have occurred in patients after SKYSONA infusion.
Important opportunistic infections that have been diagnosed within
the first 3 months after treatment with SKYSONA include BK
cystitis, cytomegalovirus reactivation, human herpesvirus-6
viremia, candidiasis, and bacteremias. Opportunistic infections
after the first 3 months include an atypical mycobacterium vascular
device infection, pseudomonas bacteremia, and Epstein-Barr virus
reactivations diagnosed as late as 18 months after treatment with
SKYSONA. Serious infections involving adenovirus include a case of
transverse myelitis at 6 months that was attributed to adenovirus
and entero/rhinovirus infection, and a fatal adenovirus infection
at 21 months in a patient with CALD progression who developed
multisystem organ failure.
Grade 3 or higher infections occurred in 21% of all patients
(12% bacterial, 3% viral, and 6% unspecified). The most common
Grade 3 or higher infections were vascular device infections (7% of
patients) diagnosed as late as 6 months after treatment with
SKYSONA, and bacteremias (6% of patients) diagnosed as late as 8
months after treatment with SKYSONA.
Febrile neutropenia developed within two weeks after SKYSONA
infusion in 72% of patients. In the event of febrile neutropenia,
evaluate for infection and manage with broad-spectrum antibiotics,
fluids, and other supportive care as medically indicated.
Monitor patients for signs and symptoms of infection before and
after SKYSONA administration and treat appropriately. Administer
prophylactic antimicrobials according to best clinical practices
and clinical guidelines.
Avoid administration of SKYSONA in patients with active
infections.
Prolonged Cytopenias
Patients may exhibit cytopenias, including pancytopenia, for
> 1 year following conditioning and SKYSONA infusion.
Grade 3 or higher cytopenias on or after Day 60 following
SKYSONA infusion occurred in 47% of patients and included low
platelet count (14%), low neutrophil count (22%), low lymphocyte
count (27%), and low hemoglobin (2%). Grade 3 cytopenias persisted
beyond Day 100 in 15% of patients and included low platelet count
(7%), low neutrophil count (9%), and low lymphocyte count (6%).
Serious adverse reactions of pancytopenia occurred in two
patients who required support with blood and platelet transfusions
as well as growth factors (G-CSF for up to 6 months and eltrombopag
for up to 14 months) after SKYSONA administration. One patient had
intercurrent parvovirus infection and his pancytopenia was ongoing
at least two years after SKYSONA administration. Pancytopenia in
the other patient was ongoing until he was diagnosed with
myelodysplastic syndrome approximately two years after SKYSONA
administration.
Monitor blood counts until normalization and assess patients for
signs and symptoms of bleeding and/or infection prior to and after
SKYSONA administration.
Delayed Platelet Engraftment
Delayed platelet engraftment has been observed with SKYSONA.
Bleeding risk is increased prior to platelet engraftment and may
continue after engraftment in patients with prolonged
thrombocytopenia; 14% of patients had a platelet count ≤ 50 × 109/L
beyond 60 days after treatment with SKYSONA.
Patients should be made aware of the risk of bleeding until
platelet recovery has been achieved. Monitor patients for
thrombocytopenia and bleeding according to standard guidelines.
Conduct frequent platelet counts until platelet engraftment and
platelet recovery are achieved. Perform blood cell count
determination and other appropriate testing whenever clinical
symptoms suggestive of bleeding arise.
Risk of Neutrophil Engraftment Failure
There is a potential risk of neutrophil engraftment failure
after treatment with SKYSONA. Neutrophil engraftment failure was
defined as failure to achieve 3 consecutive absolute neutrophil
counts (ANC) ≥ 0.5 × 109 cells/L obtained on different days by Day
43 after infusion of SKYSONA. Monitor neutrophil counts until
engraftment has been achieved. If neutrophil engraftment failure
occurs in a patient treated with SKYSONA, provide rescue treatment
with the back-up collection of CD34+ cells.
Hypersensitivity Reactions
Allergic reactions may occur with the infusion of SKYSONA. The
dimethyl sulfoxide (DMSO) in SKYSONA may cause hypersensitivity
reactions, including anaphylaxis which is potentially
life-threatening and requires immediate intervention.
Anti-retroviral Use
Patients should not take anti-retroviral medications for at
least one month prior to mobilization or the expected duration for
elimination of the medications, and until all cycles of apheresis
are completed. Anti-retroviral medications may interfere with
manufacturing of the apheresed cells.
If a patient requires anti-retrovirals for HIV prophylaxis,
mobilization and apheresis of CD34+ cells should be delayed until
HIV infection is adequately ruled out.
Laboratory Test Interference
SKYSONA affects polymerase chain reaction (PCR) assays for HIV
due to LVV provirus insertion. A PCR based assay should not be used
to screen for HIV infection in patients treated with SKYSONA as a
false positive test result is likely.
Adverse Reactions
Most common non-laboratory adverse reactions (≥ 20%): mucositis,
nausea, vomiting, febrile neutropenia, alopecia, decreased
appetite, abdominal pain, constipation, pyrexia, diarrhea,
headache, rash.
Most common Grade 3 or 4 laboratory abnormalities (≥40%):
leukopenia, lymphopenia, thrombocytopenia, neutropenia, anemia,
hypokalemia.
Vaccines
Vaccination is not recommended during the 6 weeks preceding the
start of myeloablative conditioning, and until hematological
recovery following treatment with SKYSONA. Where feasible,
administer childhood vaccinations prior to myeloablative
conditioning for SKYSONA.
Males of Reproductive Potential
Advise patients of the risks associated with mobilization and
conditioning agents. Males capable of fathering a child and their
female partners of childbearing potential should use an effective
method of contraception (intra uterine device or combination of
hormonal and barrier contraception) from start of mobilization
through at least 6 months after administration of SKYSONA.
Data are available on the risk of infertility with myeloablative
conditioning. Advise patients of the option to cryopreserve semen
before treatment if appropriate.
Please see full Prescribing Information for SKYSONA, including
BOXED WARNING and Medication Guide.
Investor Conference Call Information
bluebird bio will host a call for analysts and investors on
Monday, September 19, 2022, at 8:00 a.m. ET. Please note that there
is a new process to access the call via telephone. To register
online and receive a dial in number and unique PIN to access the
live conference call, please follow this link
https://register.vevent.com/register/BI6661b71df881495eb2148380462a257c.
The live webcast of the call may be accessed by visiting the
“Events & Presentations” page within the Investors & Media
section of the bluebird website at http://investor.bluebirdbio.com.
A replay of the webcast will be available on the bluebird website
for 90 days following the event.
About SKYSONA® (elivaldogene autotemcel), also known as
eli-cel
SKYSONA is a one-time gene therapy custom-designed to treat the
underlying cause of cerebral adrenoleukodystrophy (CALD). SKYSONA
uses ex-vivo transduction with the Lenti-D lentiviral vector (LVV)
to add functional copies of the ABCD1 gene into a patient’s own
hematopoietic stem cells (HSCs). The addition of the functional
ABCD1 gene allows patients to produce the ALD protein (ALDP), which
can then participate in the local degradation of very long-chain
fatty acids (VLCFAs). This degradation of VLCFAs is believed to
slow or possibly prevent further inflammation and
demyelination.
About bluebird bio, Inc.
bluebird bio is pursuing curative gene therapies to give
patients and their families more bluebird days. With a dedicated
focus on severe genetic diseases, bluebird has industry-leading
clinical and research programs for sickle cell disease,
beta-thalassemia and cerebral adrenoleukodystrophy and is advancing
research to apply new technologies to these and other diseases. We
custom design each of our therapies to address the underlying cause
of disease and have developed in-depth and effective analytical
methods to understand the safety of our lentiviral vector
technologies and drive the field of gene therapy forward.
Founded in 2010, bluebird has the largest and deepest ex-vivo
gene therapy data set in the world—setting the standard for
industry. Today, bluebird continues to forge new paths, combining
our real-world experience with a deep commitment to patient
communities and a people-centric culture that attracts and grows a
diverse flock of dedicated birds.
For more information, visit bluebirdbio.com or follow us
on social media at @bluebirdbio, LinkedIn,
Instagram and YouTube.
SKYSONA and bluebird bio are trademarks of bluebird bio,
Inc.
bluebird bio Cautionary Statement Regarding Forward-Looking
Statements
This press release contains “forward-looking statements” within
the meaning of the Private Securities Litigation Reform Act of
1995. All statements that are not statements of historical facts
are, or may be deemed to be, forward-looking statements, including
statements regarding the satisfaction of the post-marketing
requirement to provide confirmatory data on SKYSONA, the timing of
availability of SKYSONA as a commercial product, including the
availability at certain QTCs, and the availability of services
offered by the my bluebird support program to support patient
treatment. Such forward-looking statements are based on historical
performance and current expectations and projections about our
future goals, plans and objectives and involve inherent risks,
assumptions and uncertainties, including internal or external
factors that could delay, divert or change any of them in the next
several years, that are difficult to predict, may be beyond our
control and could cause our future goals, plans and objectives to
differ materially from those expressed in, or implied by, the
statements. No forward-looking statement can be guaranteed.
Forward-looking statements in this press release should be
evaluated together with the many risks and uncertainties that
affect bluebird bio’s business, particularly those identified in
the risk factors discussion in bluebird bio’s Annual Report on Form
10-K for the year ended December 31, 2021, as updated by our
subsequent Quarterly Reports on Form 10-Q, Current Reports on Form
8-K and other filings with the Securities and Exchange Commission.
These risks and uncertainties include, but are not limited to: the
risk that the efficacy and safety results from our prior and
ongoing clinical trials will not continue or be seen in the
commercial treatment context; the risk that additional insertional
oncogenic or other safety events associated with lentiviral vector,
drug product, or myeloablation will be discovered or reported over
time; the risk that the results of ongoing or future studies,
including LTF-304, may fail to support full approval of SKYSONA
and, if not, additional studies may be required; the risk that we
may not be able to obtain adequate price and reimbursement for any
approved products; the risk that we may encounter delays in the
initiation of our commercial operations in the United States; the
risk that we are not able to activate QTCs on the timeframe that we
expect; the risk that the QTCs experience delays in their ability
to enroll or treat patients; the risk that we experience delays in
establishing operational readiness across our supply chain
following approval to support treatment in the commercial context;
and the risk that any one or more of our product candidates will
not be successfully developed, approved by the FDA or
commercialized. The forward-looking statements included in this
press release are made only as of the date of this press release
and except as otherwise required by applicable law, bluebird bio
undertakes no obligation to publicly update or revise any
forward-looking statement, whether as a result of new information,
future events, changed circumstances or otherwise.
i Dr. David Williams, Chief of Hematology/Oncology at Boston
Children's Hospital served as a Principal Investigator for SKYSONA
clinical studies. He has consulted for bluebird bio but has not
consulted for the SKYSONA (also known as eli-cel) technology.
View source
version on businesswire.com: https://www.businesswire.com/news/home/20220916005595/en/
Investors: Courtney O’Leary, 978-621-7347
coleary@bluebirdbio.com
Media: Jess Rowlands, 857-299-6103
jess.rowlands@bluebirdbio.com
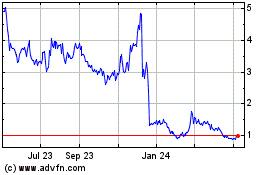
bluebird bio (NASDAQ:BLUE)
Historical Stock Chart
From Aug 2024 to Sep 2024
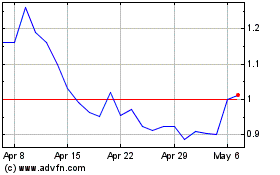
bluebird bio (NASDAQ:BLUE)
Historical Stock Chart
From Sep 2023 to Sep 2024