bluebird bio, Inc. (Nasdaq: BLUE) announced today that
data from its gene therapy programs for transfusion-dependent
β-thalassemia (TDT) and sickle cell disease (SCD) and its cell
therapy program for relapsed or refractory multiple myeloma (R/RMM)
will be presented during EHA2021 Virtual, the 26th Annual Congress
of the European Hematology Association, taking place June 9-17,
2021.
bluebird bio will present data from its ongoing clinical studies
of betibeglogene autotemcel (beti-cel), including updated results
from the Phase 3 Northstar-2 (HGB-207) and the Phase 3 Northstar-3
(HGB-212) studies, as well as long-term efficacy and safety results
from the LTF-303 follow-up study. Additionally, data from the
company’s Phase 1/2 HGB-206 study of LentiGlobin for SCD (bb1111)
will be shared.
Data from the pivotal Phase 2 KarMMa study of ABECMA®
(idecabtagene vicleucel; ide-cel) in R/RMM will also be presented
in encore presentations, in partnership with Bristol Myers Squibb,
including long-term results and a sub-analysis of characteristics
of treatment-associated neurotoxicity.
Transfusion-Dependent β-Thalassemia Data at EHA2021
Oral Presentation [S266]: Betibeglogene autotemcel in
Patients With Transfusion-Dependent β-Thalassemia: Updated Results
From HGB-207 (Northstar-2) and HGB-212 (Northstar-3) Presenting
Author: Professor Franco Locatelli, Director, Department of
Pediatric Hematology and Oncology, Ospedale Pediatrico Bambino
Gesù, Rome, Italy Session Title: Changing the Scene on
Thalassemias Date & Time: Available on Demand, Friday,
June 11; Live Q&A Session
Oral Presentation [S257]: Betibeglogene autotemcel Gene
Therapy for the Treatment of Transfusion-Dependent β-Thalassemia:
Updated Long-Term Efficacy and Safety Results Presenting
Author: Dr. Evangelia Yannaki, Director, Gene and Cell Therapy
Center, Hematology Department, George Papanicolaou Hospital,
Thessaloniki, Greece Session Title: Cellular Immunotherapy
and Gene Therapy – Clinical Date & Time: Available on
Demand, Friday, June 11; Live Q&A Session
ePoster [EP1301]: Interim Results of Betibeglogene autotemcel
Gene Therapy in Pediatric Patients with Transfusion-Dependent
β-thalassemia (TDT) Treated in the Phase 3 Northstar-2 (HGB-207)
and Northstar-3 (HGB-212) Studies Presenting Author: Dr.
Andreas E. Kulozik, Chairman, Department of Pediatric Oncology,
Hematology and Immunology, and Director, Hopp Children's Cancer
Center, University of Heidelberg, Heidelberg, Germany
ePoster [EP1309]: A Retrospective Database Study of Disease
Course and Clinical Outcomes in Patients with Transfusion-dependent
Thalassemia (TDT) in Italy Presenting Author: Dr. Angela
Vitrano, Campus of Hematology Franco and Piera Cutino, AOOR Villa
Sofia-V. Cervello, Palermo, Italy
Sickle Cell Disease Data at EHA2021
Oral Presentation [S261]: Complete Resolution of Severe
Vaso-Occlusive Events and Improved Pathophysiology with LentiGlobin
Gene Therapy in Sickle Cell Disease (SCD): Ongoing Phase 1/2
HGB-206 Group C Study Presenting Author: Dr. Janet L.
Kwiatkowski, Director, Thalassemia Center at Children's Hospital of
Philadelphia, Philadelphia, PA Session Title: Changing the
Scene on Sickle Cell Disease Date & Time: Available on
Demand, Friday, June 11; Live Q&A Session
ePoster [EP1212]: Complications of Sickle Cell Disease in
East London Newborn Cohort Patients Over the Years 2015-2018
Presenting Author: Muriel Soriano, Centre of Genomics and Child
Health, Queen Mary University of London, London, United Kingdom
Multiple Myeloma Data at EHA2021
ePoster [EP984]: Characteristics of Neurotoxicity Associated
with Idecabtagene Vicleucel (ide-cel, bb2121) in Patients with
Relapsed and Refractory Multiple Myeloma in the Pivotal Phase II
KarMMa Study Presenting Author: Dr. Salomon Manier, Department
of Hematology, Lille University Hospital, Lille, France
ePoster [EP1009]: Idecabtagene Vicleucel (ide-cel, bb2121), a
BCMA-Directed CAR T Cell Therapy, in Patients with Relapsed and
Refractory Multiple Myeloma: Updated KarMMa Results Presenting
Author: Dr. Albert Oriol, Institut Josep Carreras and Institut
Catala d’Oncologia, Hospital Germans Trias i Pujol, Badalona,
Spain
Abstracts are available on the EHA2021 conference
website.
About betibeglogene autotemcel (beti-cel)
Betibeglogene autotemcel (beti-cel) is a one-time gene therapy
that adds functional copies of a modified form of the β-globin gene
(βA-T87Q-globin gene) into a patient’s own hematopoietic (blood)
stem cells (HSCs). Once a patient has the βA-T87Q-globin gene, they
have the potential to produce HbAT87Q, which is gene
therapy-derived adult hemoglobin (Hb), at levels that may eliminate
or significantly reduce the need for transfusions. In studies of
beti-cel, transfusion independence (TI) is defined as no longer
needing red blood cell transfusions for at least 12 months while
maintaining a weighted average Hb of at least 9 g/dL.
The European Commission granted conditional marketing
authorization (CMA) for beti-cel, marketed as ZYNTEGLO™ gene
therapy, for patients 12 years and older with TDT who do not have a
β0/β0 genotype, for whom hematopoietic stem cell (HSC)
transplantation is appropriate, but a human leukocyte antigen
(HLA)-matched related HSC donor is not available. Non-serious
adverse events (AEs) observed during clinical studies that were
attributed to beti-cel included abdominal pain, thrombocytopenia,
leukopenia, neutropenia, hot flush, dyspnea, pain in extremity,
tachycardia and non-cardiac chest pain. One serious adverse event
(SAE) of thrombocytopenia was considered possibly related to
beti-cel.
Additional AEs observed in clinical studies were consistent with
the known side effects of HSC collection and bone marrow ablation
with busulfan, including SAEs of veno-occlusive disease. For
details, please see the Summary of Product Characteristics
(SmPC).
On April 28, 2020, the European Medicines Agency (EMA) renewed
the CMA for beti-cel. The CMA for beti-cel is valid in the 27
member states of the EU as well as the UK, Iceland, Liechtenstein
and Norway. In November 2020, bluebird bio submitted to the EMA an
application for the second renewal of the CMA. This procedure is
currently on hold while the EMA's Pharmacovigilance Risk Assessment
Committee (PRAC) reviews the safety of ZYNTEGLO. The CMA is valid
while the renewal application review is ongoing and while it is on
hold by the regulatory agency. The U.S. Food and Drug
Administration (FDA) granted beti-cel Orphan Drug status and
Breakthrough Therapy designation for the treatment of TDT. Beti-cel
is not approved in the U.S.
Beti-cel continues to be evaluated in the ongoing Phase 3
Northstar-2 (HGB-207) and Northstar-3 (HGB-212) studies, which are
on clinical hold. bluebird bio is conducting a long-term safety and
efficacy follow-up study, LTF-303, for people who have participated
in bluebird bio-sponsored clinical studies of beti-cel.
About LentiGlobin for SCD (bb1111)
LentiGlobin gene therapy for sickle cell disease (bb1111) is an
investigational treatment being studied as a potential treatment
for SCD. bluebird bio’s clinical development program for
LentiGlobin for SCD includes the completed Phase 1/2 HGB-205 study.
It also includes the Phase 1/2 HGB-206 and the Phase 3 HGB-210
studies, which are on clinical hold.
The U.S. FDA granted orphan drug designation, fast track
designation, regenerative medicine advanced therapy (RMAT)
designation and rare pediatric disease designation for LentiGlobin
for SCD.
LentiGlobin for SCD received orphan medicinal product
designation from the European Commission for the treatment of SCD,
and Priority Medicines (PRIME) eligibility by the EMA in September
2020.
bluebird bio is conducting a long-term safety and efficacy
follow-up study (LTF-307) for people who have participated in
bluebird bio-sponsored clinical studies of LentiGlobin for SCD. For
more information visit:
https://www.bluebirdbio.com/our-science/clinical-trials or
clinicaltrials.gov and use identifier NCT04628585 for
LTF-307.
LentiGlobin for SCD is investigational and has not been approved
in any geography.
About ABECMA®
ABECMA is the first-in-class B-cell maturation antigen
(BCMA)-directed chimeric antigen receptor (CAR) T cell
immunotherapy approved in the U.S. for the treatment of adult
patients with relapsed and refractory multiple myeloma after four
or more prior lines of therapy, including and immunomodulatory
agent, a proteasome inhibitor, and an anti-CD38 monoclonal
antibody. ABECMA recognizes and binds to BCMA on the surface of
multiple myeloma cells leading to CAR T cell proliferation,
cytokine secretion, and subsequent cytolytic killing of
BCMA-expressing cells. ABECMA is being jointly developed and
commercialized in the U.S. as part of a Co-Development,
Co-Promotion, and Profit Share Agreement with Bristol Myers Squibb
and bluebird bio.
Bristol Myers Squibb and bluebird bio’s broad clinical
development program for ABECMA includes clinical studies (KarMMa-2,
KarMMa-3, KarMMa-4, KarMMa-7) in earlier lines of treatment for
patients with multiple myeloma, including newly diagnosed multiple
myeloma. For more information visit clinicaltrials.gov.
Indication
ABECMA (idecabtagene vicleucel) is a B-cell maturation antigen
(BCMA)-directed genetically modified autologous T cell
immunotherapy indicated for the treatment of adult patients with
relapsed or refractory multiple myeloma after four or more prior
lines of therapy, including an immunomodulatory agent, a proteasome
inhibitor, and an anti-CD38 monoclonal antibody.
Important Safety Information
BOXED WARNING: CYTOKINE RELEASE SYNDROME, NEUROLOGIC
TOXICITIES, HLH/MAS, AND PROLONGED CYTOPENIA
- Cytokine Release Syndrome (CRS), including fatal or
life-threatening reactions, occurred in patients following
treatment with ABECMA. Do not administer ABECMA to patients with
active infection or inflammatory disorders. Treat severe or
life-threatening CRS with tocilizumab or tocilizumab and
corticosteroids.
- Neurologic Toxicities, which may be severe or life-threatening,
occurred following treatment with ABECMA, including concurrently
with CRS, after CRS resolution, or in the absence of CRS. Monitor
for neurologic events after treatment with ABECMA. Provide
supportive care and/or corticosteroids as needed.
- Hemophagocytic Lymphohistiocytosis/Macrophage Activation
Syndrome (HLH/MAS) including fatal and life-threatening reactions,
occurred in patients following treatment with ABECMA. HLH/MAS can
occur with CRS or neurologic toxicities.
- Prolonged Cytopenia with bleeding and infection, including
fatal outcomes following stem cell transplantation for
hematopoietic recovery, occurred following treatment with
ABECMA.
- ABECMA is available only through a restricted program under a
Risk Evaluation and Mitigation Strategy (REMS) called the ABECMA
REMS.
Cytokine Release Syndrome (CRS): CRS, including fatal or
life-threatening reactions, occurred following treatment with
ABECMA. CRS occurred in 85% (108/127) of patients receiving ABECMA.
Grade 3 or higher CRS (Lee grading system) occurred in 9% (12/127)
of patients, with Grade 5 CRS reported in one (0.8%) patient. The
median time to onset of CRS, any grade, was 1 day (range: 1 - 23
days) and the median duration of CRS was 7 days (range: 1 - 63
days) in all patients including the patient who died. The most
common manifestations of CRS included pyrexia (98%), hypotension
(41%), tachycardia (35%), chills (31%), hypoxia (20%), fatigue
(12%), and headache (10%). Grade 3 or higher events that may be
associated with CRS include hypotension, hypoxia,
hyperbilirubinemia, hypofibrinogenemia, acute respiratory distress
syndrome (ARDS), atrial fibrillation, hepatocellular injury,
metabolic acidosis, pulmonary edema, multiple organ dysfunction
syndrome and HLH/MAS.
Identify CRS based on clinical presentation. Evaluate for and
treat other causes of fever, hypoxia, and hypotension. CRS has been
reported to be associated with findings of HLH/MAS, and the
physiology of the syndromes may overlap. HLH/MAS is a potentially
life-threatening condition. In patients with progressive symptoms
of CRS or refractory CRS despite treatment, evaluate for evidence
of HLH/MAS.
Fifty four percent (68/127) of patients received tocilizumab;
35% (45/127) received a single dose while 18% (23/127) received
more than 1 dose of tocilizumab. Overall, across the dose levels,
15% (19/127) of patients received at least 1 dose of
corticosteroids for treatment of CRS. All patients that received
corticosteroids for CRS received tocilizumab.
Overall rate of CRS was 79% and rate of Grade 2 CRS was 23% in
patients treated in the 300 x 106 CAR+ T cell dose cohort. For
patients treated in the 450 x 106 CAR+ T cell dose cohort, the
overall rate of CRS was 96% and rate of Grade 2 CRS was 40%. Rate
of Grade 3 or higher CRS was similar across the dose range. The
median duration of CRS for the 450 x 106 CAR+ T cell dose cohort
was 7 days (range: 1-63 days) and for the 300 x 106 CAR+ T cell
dose cohort was 6 days (range: 2-28 days). In the 450 x 106 CAR+ T
cell dose cohort, 68% (36/53) of patients received tocilizumab and
23% (12/53) received at least 1 dose of corticosteroids for
treatment of CRS. In the 300 x 106 CAR+ T cell dose cohort, 44%
(31/70) of patients received tocilizumab and 10% (7/70) received
corticosteroids. All patients that received corticosteroids for CRS
also received tocilizumab. Ensure that a minimum of 2 doses of
tocilizumab are available prior to infusion of ABECMA.
Monitor patients at least daily for 7 days following ABECMA
infusion at the REMS-certified healthcare facility for signs and
symptoms of CRS. Monitor patients for signs or symptoms of CRS for
at least 4 weeks after infusion. At the first sign of CRS,
institute treatment with supportive care, tocilizumab and/or
corticosteroids as indicated.
Counsel patients to seek immediate medical attention should
signs or symptoms of CRS occur at any time.
Neurologic Toxicities: Neurologic toxicities, which may
be severe or life-threatening, occurred following treatment with
ABECMA, including concurrently with CRS, after CRS resolution, or
in the absence of CRS. CAR T cell-associated neurotoxicity occurred
in 28% (36/127) of patients receiving ABECMA, including Grade 3 in
4% (5/127) of patients. One patient had ongoing Grade 2
neurotoxicity at the time of death. Two patients had ongoing Grade
1 tremor at the time of data cutoff. The median time to onset of
neurotoxicity was 2 days (range: 1 - 42 days). CAR T
cell-associated neurotoxicity resolved in 92% (33/36) of patients
with a median duration of neurotoxicity was 5 days (range: 1 - 61
days). The median duration of neurotoxicity was 6 days (range: 1 -
578) in all patients including those with ongoing neurotoxicity at
the time of death or data cut off. Thirty-four patients with
neurotoxicity had CRS. Neurotoxicity had onset in 3 patients
before, 29 patients during, and 2 patients after CRS. The rate of
Grade 3 neurotoxicity was 8% in the 450 x 106 CAR+ T cell dose
cohort and 1.4% in the 300 x 106 CAR+ T cell dose cohort. The most
frequently reported (greater than or equal to 5%) manifestations of
CAR T cell-associated neurotoxicity include encephalopathy (20%),
tremor (9%), aphasia (7%), and delirium (6%). Grade 4 neurotoxicity
and cerebral edema in 1 patient has been reported with ABECMA in
another study in multiple myeloma. Grade 3 myelitis and Grade 3
parkinsonism have been reported after treatment with ABECMA in
another study in multiple myeloma.
Monitor patients at least daily for 7 days following ABECMA
infusion at the REMS-certified healthcare facility for signs and
symptoms of neurologic toxicities. Rule out other causes of
neurologic symptoms. Monitor patients for signs or symptoms of
neurologic toxicities for at least 4 weeks after infusion and treat
promptly. Neurologic toxicity should be managed with supportive
care and/or corticosteroids as needed.
Counsel patients to seek immediate medical attention should
signs or symptoms of neurologic toxicity occur at any time.
Hemophagocytic Lymphohistiocytosis (HLH)/Macrophage
Activation Syndrome (MAS): HLH/MAS occurred in 4% (5/127) of
patients receiving ABECMA. One patient treated in the 300 x 106
CAR+ T cell dose cohort developed fatal multi-organ HLH/MAS with
CRS. In another patient with fatal bronchopulmonary aspergillosis,
HLH/MAS was contributory to the fatal outcome. Three cases of Grade
2 HLH/MAS resolved. The rate of HLH/MAS was 8% in the 450 x 106
CAR+ T cell dose cohort and 1% in the 300 x 106 CAR+ T cell dose
cohort. All events of HLH/MAS had onset within 10 days of receiving
ABECMA with a median onset of 7 days (range: 4-9 days) and occurred
in the setting of ongoing or worsening CRS. Two patients with
HLH/MAS had overlapping neurotoxicity. The manifestations of
HLH/MAS include hypotension, hypoxia, multiple organ dysfunction,
renal dysfunction, and cytopenia. HLH/MAS is a potentially
life-threatening condition with a high mortality rate if not
recognized early and treated. Treatment of HLH/MAS should be
administered per institutional standards.
ABECMA REMS: Due to the risk of CRS and neurologic
toxicities, ABECMA is available only through a restricted program
under a Risk Evaluation and Mitigation Strategy (REMS) called the
ABECMA REMS. Further information is available at
www.AbecmaREMS.com or 1‑888‑423‑5436.
Hypersensitivity Reactions: Allergic reactions may occur
with the infusion of ABECMA. Serious hypersensitivity reactions,
including anaphylaxis, may be due to dimethyl sulfoxide (DMSO) in
ABECMA.
Infections: ABECMA should not be administered to patients
with active infections or inflammatory disorders. Severe,
life-threatening, or fatal infections occurred in patients after
ABECMA infusion. Infections (all grades) occurred in 70% of
patients. Grade 3 or 4 infections occurred in 23% of patients.
Overall, 4 patients had Grade 5 infections (3%); 2 patients (1.6%)
had Grade 5 events of pneumonia, 1 patient (0.8%) had Grade 5
bronchopulmonary aspergillosis, and 1 patient (0.8%) had
cytomegalovirus (CMV) pneumonia associated with Pneumocystis
jirovecii. Monitor patients for signs and symptoms of infection
before and after ABECMA infusion and treat appropriately.
Administer prophylactic, preemptive, and/or therapeutic
antimicrobials according to standard institutional guidelines.
Febrile neutropenia was observed in 16% (20/127) of patients after
ABECMA infusion and may be concurrent with CRS. In the event of
febrile neutropenia, evaluate for infection and manage with broad
spectrum antibiotics, fluids, and other supportive care as
medically indicated.
Viral Reactivation: Cytomegalovirus (CMV) infection resulting in
pneumonia and death has occurred following ABECMA administration.
Monitor and treat for CMV reactivation in accordance with clinical
guidelines. Hepatitis B virus (HBV) reactivation, in some cases
resulting in fulminant hepatitis, hepatic failure, and death, can
occur in patients treated with drugs directed against plasma cells.
Perform screening for CMV, HBV, hepatitis C virus (HCV), and human
immunodeficiency virus (HIV) in accordance with clinical guidelines
before collection of cells for manufacturing.
Prolonged Cytopenias: Patients may exhibit prolonged
cytopenias following lymphodepleting chemotherapy and ABECMA
infusion. In the KarMMa study, 41% of patients (52/127) experienced
prolonged Grade 3 or 4 neutropenia and 49% (62/127) experienced
prolonged Grade 3 or 4 thrombocytopenia that had not resolved by
Month 1 following ABECMA infusion. Rate of prolonged neutropenia
was 49% in the 450 x 106 CAR+ T cell dose cohort and 34% in the 300
x 106 CAR+ T cell dose cohort. In 83% (43/52) of patients who
recovered from Grade 3 or 4 neutropenia after Month 1, the median
time to recovery from ABECMA infusion was 1.9 months. In 65%
(40/62) of patients who recovered from Grade 3 or 4
thrombocytopenia, the median time to recovery was 2.1 months.
Median time to cytopenia recovery was similar across the 300 and
450 x 106 dose cohort.
Three patients underwent stem cell therapy for hematopoietic
reconstitution due to prolonged cytopenia. Two of the three
patients died from complications of prolonged cytopenia. Monitor
blood counts prior to and after ABECMA infusion. Manage cytopenia
with myeloid growth factor and blood product transfusion support
according to institutional guidelines.
Hypogammaglobulinemia: Plasma cell aplasia and
hypogammaglobulinemia can occur in patients receiving treatment
with ABECMA. Hypogammaglobulinemia was reported as an adverse event
in 21% (27/127) of patients; laboratory IgG levels fell below 500
mg/dl after infusion in 25% (32/127) of patients treated with
ABECMA.
Monitor immunoglobulin levels after treatment with ABECMA and
administer IVIG for IgG <400 mg/dl. Manage per local
institutional guidelines, including infection precautions and
antibiotic or antiviral prophylaxis.
The safety of immunization with live viral vaccines during or
following ABECMA treatment has not been studied. Vaccination with
live virus vaccines is not recommended for at least 6 weeks prior
to the start of lymphodepleting chemotherapy, during ABECMA
treatment, and until immune recovery following treatment with
ABECMA.
Secondary Malignancies: Patients treated with ABECMA may
develop secondary malignancies. Monitor life-long for secondary
malignancies. If a secondary malignancy occurs, contact Bristol
Myers Squibb at 1-888-805-4555 to obtain instructions on patient
samples to collect for testing of secondary malignancy of T cell
origin.
Effects on Ability to Drive and Operate Machinery: Due to
the potential for neurologic events, including altered mental
status or seizures, patients receiving ABECMA are at risk for
altered or decreased consciousness or coordination in the 8 weeks
following ABECMA infusion. Advise patients to refrain from driving
and engaging in hazardous occupations or activities, such as
operating heavy or potentially dangerous machinery, during this
initial period.
Adverse Reactions: The most common nonlaboratory adverse
reactions (incidence greater than or equal to 20%) include CRS,
infections – pathogen unspecified, fatigue, musculoskeletal pain,
hypogammaglobulinemia, diarrhea, upper respiratory tract infection,
nausea, viral infections, encephalopathy, edema, pyrexia, cough,
headache, and decreased appetite.
Please see full Prescribing Information, including
Boxed WARNINGS and Medication Guide.
About bluebird bio, Inc.
bluebird bio is pioneering gene therapy with purpose. From our
Cambridge, Mass., headquarters, we’re developing gene and cell
therapies for severe genetic diseases and cancer, with the goal
that people facing potentially fatal conditions with limited
treatment options can live their lives fully. Beyond our labs,
we’re working to positively disrupt the healthcare system to create
access, transparency and education so that gene therapy can become
available to all those who can benefit.
bluebird bio is a human company powered by human stories. We’re
putting our care and expertise to work across a spectrum of
disorders including cerebral adrenoleukodystrophy, sickle cell
disease, β-thalassemia and multiple myeloma using three gene
therapy technologies: gene addition, cell therapy and
(megaTAL-enabled) gene editing.
bluebird bio has additional nests in Seattle, Wash.; Durham,
N.C.; and Zug, Switzerland. For more information, visit
bluebirdbio.com.
Follow bluebird bio on social media: @bluebirdbio,
LinkedIn, Instagram and YouTube.
ZYNTEGLO, betibeglogene autotemcel, beti-cel, and bluebird bio
are trademarks of bluebird bio, Inc.
bluebird bio Cautionary Statement Regarding Forward-Looking
Statements
This press release contains “forward-looking statements” within
the meaning of the Private Securities Litigation Reform Act of
1995. All statements that are not statements of historical facts
are, or may be deemed to be, forward-looking statements. Such
forward-looking statements are based on historical performance and
current expectations and projections about our future financial
results, goals, plans and objectives and involve inherent risks,
assumptions and uncertainties, including internal or external
factors that could delay, divert or change any of them in the next
several years, that are difficult to predict, may be beyond our
control and could cause our future financial results, goals, plans
and objectives to differ materially from those expressed in, or
implied by, the statements. No forward-looking statement can be
guaranteed. Forward-looking statements in this press release should
be evaluated together with the many risks and uncertainties that
affect bluebird bio’s business, particularly those identified in
the risk factors discussion in bluebird bio’s Annual Report on Form
10-K, as updated by our subsequent Quarterly Reports on Form 10-Q,
Current Reports on Form 8-K and other filings with the Securities
and Exchange Commission. The forward-looking statements included in
this document are made only as of the date of this document and
except as otherwise required by applicable law, bluebird bio
undertakes no obligation to publicly update or revise any
forward-looking statement, whether as a result of new information,
future events, changed circumstances or otherwise.
Hyperlinks are provided as a convenience and for informational
purposes only. Neither Bristol Myers Squibb nor bluebird bio bears
responsibility for the security or content of external websites or
websites outside of their respective control.
View source
version on businesswire.com: https://www.businesswire.com/news/home/20210513005568/en/
Investors: Elizabeth Pingpank, 617-914-8736
epingpank@bluebirdbio.com
or
Media: Catherine Falcetti, 617-583-3411
cfalcetti@bluebirdbio.com
Victoria von Rinteln, 617-914-8774
vvonrinteln@bluebirdbio.com
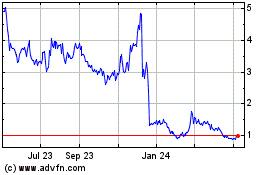
bluebird bio (NASDAQ:BLUE)
Historical Stock Chart
From Aug 2024 to Sep 2024
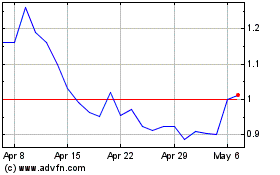
bluebird bio (NASDAQ:BLUE)
Historical Stock Chart
From Sep 2023 to Sep 2024