Seamless Data Exchange Improves Patient Access
to Care, Reduces Administrative Burden Across the Healthcare
Ecosystem
athenahealth, a leading provider of network-enabled software and
services for medical groups and health systems nationwide along
with collaborators Availity, Harmony Park Family Medicine, and
Humana (NYSE: HUM), received a 2024 Points of Light Award from
KLAS. The group’s case study, “Using FHIR Standards to Streamline
Prior Authorization Management & Improve Patient Care,”
recognized the organizations’ work together to modernize the prior
authorization process and expedite approval of prior authorization
requests.
This press release features multimedia. View
the full release here:
https://www.businesswire.com/news/home/20240604470805/en/
(Graphic: Business Wire)
Prior authorization is the process used to obtain insurance
approval for medications and certain medical procedures before they
can be performed. It is designed to ensure that patients receive
timely, clinically appropriate, evidence-based care. This
collaboration aims to deliver an end-to-end process that
streamlines, automates, and reduces administrative burdens to the
benefit of all parties involved.
“Our mission is to ensure that our members can get the
high-quality, affordable care they need while delivering the better
health outcomes they deserve,” said Angie Shaw, Humana’s Vice
President of Clinical Operations Shared Services. “By partnering
with athenahealth, Availity, and Harmony Park, as well as others in
the industry, we are working to streamline the prior authorization
process in ways that improve patient access to care and deliver
better health outcomes.”
Humana, Availity, and athenahealth worked together to develop an
automated electronic prior authorization (EPA) process leveraging
the Da Vinci Burden Reduction Implementation Guides – a set of
standards designed to make the process of prior authorization in
healthcare more efficient and streamlined – to expedite approval of
these requests and deliver a better, more seamless end-to-end
experience for patients, providers, and payers.
One of the key achievements of the project was Availity creating
a seamless data exchange to connect the Humana and athenahealth
platforms, allowing data to be effortlessly exchanged. “Unlike many
healthcare transactions, prior authorization is not always a simple
query and response but can be a complex conversation, and that’s
why we’re working to improve this process for beneficiaries,
providers and payers," said Russ Thomas, CEO of Availity. “We are
proud to be recognized for our collaboration with athenahealth,
Harmony Park, and Humana.”
The EPA process has saved Harmony Park 24 hours per week in
manual work that can now be redirected to patient-centric
activities. “With this new automated prior authorization process
enabled within the athenahealth EHR, our providers now have all
necessary information and requests directly within their workflow,”
said Yvonne Dooley, Chief Operating Officer, Harmony Park Family
Medicine, a provider in Hot Springs, Arkansas that is successfully
using the tool. “This, combined with the speed and transparency we
now have throughout the entire process, has greatly reduced
administrative burden for our staff, and patients are able to
receive care more quickly in anticipation of improved health
outcomes.”
Key outcomes of the collaboration, detailed in the case study,
include quicker patient access to care, improved provider
efficiency, and decreased administrative burden as compared to when
the workflow is entirely manual. Stakeholders determined that
during the evaluation period, nearly 54% of all requests per month
required no authorization, and 70% of prior authorization requests
processed through the implementation were instantly approved by
Humana, due to the integration that enables robust data gathering
and sharing. These instant approvals have contributed to a dramatic
reduction in turnaround time from multiple days to about one day,
which far exceeds industry averages that range from days to weeks
and the seven-day target established by the CMS Interoperability
and Prior Authorization Final Rule.
“At athenahealth, we take on and automate time-consuming, manual
tasks so that practice staff can focus on supporting patients,”
said Paul Brient, Chief Product Officer at athenahealth. “We are
thrilled to work with our partners and customers to modernize the
process associated with prior authorization. This type of industry
collaboration can simplify the practice of care and drive
meaningful improvements for providers, patients, and payers.”
The KLAS Points of Light annual awards celebrate success stories
achieved by payers, healthcare organizations, and healthcare IT
companies who have partnered to reduce costs and inefficiencies and
improve the patient experience. The awards were presented at the
KLAS K2 Collaborative Summit, May 14-15 in Salt Lake City.
To learn more about the challenges, outcomes, and key lessons
from this collaboration, please visit:
https://www.athenahealth.com/KLAS-POL-2024.
About athenahealth
athenahealth strives to cure complexity and simplify the
practice of healthcare. Our innovative technology includes
electronic health records, revenue cycle management, and patient
engagement solutions that help healthcare providers,
administrators, and practices eliminate friction for patients while
getting paid efficiently. athenahealth partners with practices with
purpose-built software backed by expertise to produce the insights
needed to drive better clinical and financial outcomes. We’re
inspired by our vision to create a thriving ecosystem that delivers
accessible, high-quality, and sustainable healthcare for all. Learn
more at athenahealth.com.
About Humana
Humana Inc. is committed to putting health first – for our
teammates, our customers, and our company. Through our Humana
insurance services, and our CenterWell health care services, we
make it easier for the millions of people we serve to achieve their
best health – delivering the care and service they need, when they
need it. These efforts are leading to a better quality of life for
people with Medicare, Medicaid, families, individuals, military
service personnel, and communities at large. Learn more about what
we offer at Humana.com and at CenterWell.com.
About Availity
Availity is the trusted partner for organizations seeking to
realize the greatest value from clinical, administrative, and
financial data. Positioned at the nexus of provider, health plan,
and consumer health information, Availity develops scalable,
innovative solutions for healthcare data acquisition,
standardization, transparency, automation, and exchange among
health plans, providers, and technology partners. As one of the
nation's largest health information networks, Availity facilitates
billions of clinical, administrative, and financial transactions
annually. Our suite of dynamic products, built on a powerful,
intelligent platform, enables real-time collaboration for success
in a competitive, value-based care environment.
For more information, including an online demonstration, please
visit www.availity.com or call 1.800.AVAILITY (282.4548). Follow us
on LinkedIn and X.
About Harmony Park Family Medicine
Harmony Park Family Medicine, located in Hot Springs, AR, is
committed to offering professional, compassionate, and coordinated
patient care. Harmony Park provides patient-centric care, wellness
services, and a specialized chronic care management program, as
well as convenient online portal access to appointment scheduling,
health records and results, and online bill payment. Learn more at
harmonyparkfamilymedicine.com.
View source
version on businesswire.com: https://www.businesswire.com/news/home/20240604470805/en/
Media contact: Jean Borgman jborgman@athenahealth.com
Humana: Kevin Smith Ksmith305@humana.com
Availity: Matt Schlossberg Matt.schlossberg@availity.com
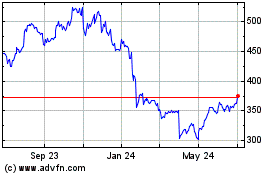
Humana (NYSE:HUM)
Historical Stock Chart
From Jun 2024 to Jul 2024
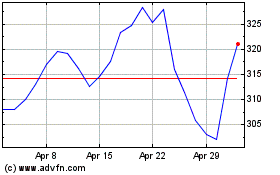
Humana (NYSE:HUM)
Historical Stock Chart
From Jul 2023 to Jul 2024