EnvisionRx Prioritizes Opioid Safety with Multi-Faceted Pain Management Program
May 17 2018 - 11:26AM
Business Wire
Pharmacy benefit manager’s enhanced program
helps payers safely address members' pain and lower risk of
abuse
Program helps educate and guide patients
prescribed opioids to safely use these powerful drugs
In response to the nation’s opioid epidemic, pharmacy benefit
manager, EnvisionRx, a division of
EnvisionRxOptions, announced enhancements to its comprehensive
opioid and pain management program, EnvisionCare Pain Management.
Available immediately, the program includes pre-emptive
prescription strategies, such as limiting first-time fills to seven
days*, prior authorizations on certain medications, and shortened
windows to refill prescriptions. This comprehensive program aligns
with the healthcare company’s overall pain management strategy, as
well as the guidelines set by the Centers for Disease Control and
Prevention (CDC).
“As our nation endures a health crisis around opioid dependency,
we are in a unique position to change the way opioids are used by
our members,” explained Frank Sheehy, chief executive officer of
EnvisionRxOptions. “Prescription fill limits and monitoring as a
part of our pain management program will help minimize the risk of
opioid addiction, especially for those patients who are being
prescribed opioids for the first time.”
EnvisionCare Pain Management, which includes an opt-out feature
for clients not wishing to implement this program, focuses on
patient safety through communication, education and outreach, as
well as interventions that avoid excessive dosing and dangerous
drug combinations, ensuring pain is managed safely before and after
the first dose.
The program contains pre-dispense, concurrent and retrospective
measures, such as:
- Clinically focused safeguards, like a
seven-day limit on prescriptions for patients who have not used an
opioid in the past three months, step therapy for extended-release
opioids and prior authorization for extremely high dosages (greater
than 200 Morphine Milligram Equivalents (MME)).
- Safer dispensing practices, including
real-time drug utilization reviews at the pharmacy to promote
proper dispensing and point-of-sale alerts for excessively high
dosages or those who have been prescribed dangerous drug
combinations.
- Supplemental, detailed reviews, in
addition to those the pharmacist performs at the time of dispense,
to identify patients who may be filling high dosage opioids, and/or
receiving prescriptions from multiple prescribers and dispensers.
These reviews, paired with a shortened refill window requiring
patients to have exhausted 85% of their medication supply before a
refill will be dispensed, help identify dangerous long-term
utilization and members who may be in need of intervention.
Programs like these that include controls from before the first
dose to retrospective reviews have shown impressive results, such
as an annual 42% reduction in the number of opioids filled and a
cost reduction of nearly 30%.[1] Additionally, these programs help
control indirect costs, such as absenteeism, presenteeism, and
added medical expenses due to opioid abuse, which studies show
account for eight times more direct healthcare costs than those of
non-abusers.[2]
“We firmly believe that by reducing the number of opioids in the
hands of a new patient right from the start, we can significantly
decrease the possibility of dependence and addiction,” stated
Sheehy. “While opioid use can have positive results for pain
management, we have a responsibility to protect our members by
addressing pain in an appropriate way and better educating patients
about the risks accompanying opioids."
____________
* Member requested adjustments to this days’ supply limitation
are subject to prescriber review and direction through the prior
authorization process.
[1] EnvisionRx internal reports (2018). [2] Fudin (2015). The
economics of opioids: Abuse, REMS and treatment benefits. American
Journal of Managed Care, Vol 21, No 9. August 2015.
About EnvisionRxOptions and EnvisionRx
A wholly owned subsidiary of Rite Aid, EnvisionRxOptions is a
pharmacy services and healthcare company with a visibly different
approach to pharmacy benefits. The company’s pharmacy benefit
manager (PBM), EnvisionRx, is URAC-accredited for Pharmacy
Benefit Management and Drug Therapy Management (DTM). The first PBM
to offer true transparency, EnvisionRx provides flexible,
customizable services, such as traditional and pass-through
pricing, unique network and formulary design, and specialty
pharmacy care. Using its proprietary EnvisionCare model, EnvisionRx
optimizes all aspects of the pharmacy care experience to
consistently achieve better patient and plan outcomes. For more
information, visit envisionrx.com.
View source
version on businesswire.com: https://www.businesswire.com/news/home/20180517005997/en/
EnvisionRxOptionsBobby Creek,
813-690-8503bcreek@envisionrx.com
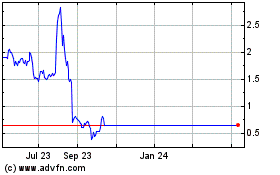
Rite Aid (NYSE:RAD)
Historical Stock Chart
From Aug 2024 to Sep 2024
Rite Aid (NYSE:RAD)
Historical Stock Chart
From Sep 2023 to Sep 2024