– LentiGlobinTM drug product manufactured with
process 2 for two patients in HGB-206 and HGB-207 confirms
two-to-threefold increase in vector copy numbers (VCNs) observed in
retrospective in vitro analyses of patients’ transduced cells ––
Company to host event at ASH with live webcast, Monday, December 5
at 8:30 p.m. PT –
bluebird bio, Inc. (Nasdaq: BLUE), a clinical-stage company
committed to developing potentially transformative gene therapies
for severe genetic diseases and T cell-based immunotherapies for
cancer, provided updates across its hematopoietic stem cell (HSC)
gene therapy programs, including:
- Updated interim clinical data from the
Northstar (HGB-204) study of LentiGlobin drug product in
transfusion-dependent β-thalassemia (TDT) confirm patients with
non-β0/β0 genotypes and ≥12 months of follow-up have stopped
regular transfusions; patients with β0/β0 genotypes and ≥12 months
of follow-up had a median reduction in transfusion volume of
63%
- Drug product vector copy numbers (DP
VCNs) for the first HGB-207 and HGB-206 patients who will be
treated using LentiGlobin drug product made using our improved
manufacturing process (process 2) are 2.9 and 3.3,
respectively
- Updated interim clinical data from
seven subjects in the HGB-206 study of LentiGlobin drug product in
severe sickle cell disease (SCD) underscore the need for recently
implemented protocol amendments seeking to improve HbAT87Q
production in this population
- Company to expand enrollment in
Starbeam study of Lenti-DTM in cerebral adrenoleukodystrophy (CALD)
by eight patients
“Our focus is learning, adjusting and implementing to innovate
on behalf of the patients we aim to serve. This year we have made
tremendous progress against this objective,” said Nick Leschly,
chief bluebird. “In 2016, we focused on further enhancing our
LentiGlobin programs in TDT and SCD by implementing high potential
manufacturing and protocol amendments while advancing our lead
bb2121 oncology program and commercialization capabilities. We are
encouraged by the data presented at ASH and how that has informed
our plans for 2017.”
TDT Program UpdatesThe
company announced that the first patient has been enrolled in
Northstar-2 (HGB-207), a Phase 3, global, multi-center study in
patients with TDT with non-β0/β0 genotypes. This study uses
LentiGlobin drug product manufactured with updated processes using
transduction enhancers. LentiGlobin DP VCN for the first patient to
be treated in Northstar-2 is 2.9 vector copies per diploid genome
(c/dg), with 77% of the stem cells lentiviral vector positive
(LVV+).
Interim data from the Northstar study were highlighted today in
an oral presentation by Alexis Thompson, M.D., M.P.H., head of the
hematology section of the Division of Hematology Oncology
Transplantation and Director of the Comprehensive Thalassemia
Program at the Ann and Robert H. Lurie Children’s Hospital of
Chicago, where she also serves as the A. Watson and Sarah Armour
Endowed Chair for Childhood Cancer and Blood Disorders.
LentiGlobin Gene Therapy for Transfusion-Dependent
β-Thalassemia: Update from the Northstar (HGB-204) Phase 1/2
Clinical Study (Abstract #1175)
The Northstar Study is an ongoing, open-label, single-dose,
international, multicenter Phase 1/2 study designed to evaluate the
safety and efficacy of LentiGlobin drug product for the treatment
of subjects with TDT. Results as of September 16, 2016 include:
- Ten patients with non-β0/β0 genotypes
and eight patients with β0/β0 genotypes have received LentiGlobin
drug product. The median follow-up was 17 months (range: 6.3 – 29.8
months); two patients have completed the two-year primary analysis
period.
- The median DP VCN for patients with
non-β0/β0 genotypes was 0.8 c/dg (range: 0.3 – 1.1 c/dg); for
patients with β0/β0 genotypes, the median DP VCN was 0.7 c/dg
(range: 0.3 – 1.5 c/dg). The median cell dose for
patients with non-β0/β0 genotypes was 7.1 x 106 CD34+
cells/kg (range: 5.2 – 13.0 x 106 cells/kg); for patients with
β0/β0 genotypes, the median cell dose was
11.0 x 106 CD34+ cells/kg (range: 6.1 – 18.1 x 106
cells/kg).
- The median in vivo VCN at six months of
follow-up was 0.4 c/dg (range 0.1-0.9 c/dg, n=10) in patients with
non-β0/β0 genotypes and 0.3 c/dg (range 0.1-1.0 c/dg, n=8) in
patients with β0/β0 genotypes.
- All patients with non-β0/β0 genotypes
with ≥12 months of follow-up (n=5) have stopped regular
transfusions (median total hemoglobin: 11.7 g/dL; range: 9.5 – 12.5
g/dL). At last follow-up, the median total hemoglobin of all
patients (n=10) with non-β0/β0 genotypes (median follow up: 14.7
months; range: 6.3 – 29.8 months) was 10.3 g/dL (range: 7.2 – 12.5
g/dl).
- Patients with β0/ β0 genotypes and ≥12
months of follow-up had a median reduction in annualized
transfusion volume of 63% (range 47 – 78%) and median reduction in
annualized transfusion frequency of 65% (range 31 – 81%),
calculated based on their transfusion requirements from month 6 to
data cut-off. The median follow-up was 17.3 months (range: 6.7 –
25.4 months). Hemoglobin fractions at month 12 show consistent
production of HbAT87Q across genotypes ≥12 months of
follow-up.
- A correlation between VCN and HbAT87Q
production was observed.
- The safety profile remains consistent
with myeloablative conditioning using single agent busulfan with no
≥ Grade 3 drug product-related adverse events (AEs) reported.
“The maturing interim data from the Northstar study support the
potential for LentiGlobin to provide a transformative treatment
option for patients with TDT by reducing or eliminating the
burdensome cycle of chronic blood transfusions and iron chelation,”
said David Davidson, chief medical officer, bluebird bio. “In
addition, we are pleased by the robust vector copy number and high
proportion of LVV+ CD34+ stem cells in the drug product
manufactured using transduction enhancers for the first patient to
be treated in the Phase 3 Northstar-2 study. If the clinical
correlation between drug product VCN and hemoglobin production
observed in the Northstar study continues with drug product
manufactured utilizing process 2, we are hopeful that LentiGlobin
drug product with higher VCNs will consistently yield clinically
meaningful outcomes for patients with TDT across all
genotypes.”
Severe Sickle Cell Disease Program
Updatesbluebird bio has amended the protocol of the
ongoing HGB-206 study in patients with severe SCD to incorporate
several changes with the goal of increasing production of HbAT87Q,
such as increasing the percentage of transduced cells through
manufacturing improvements, increasing target busulfan area under
the curve (AUC), introducing a minimum period of regular blood
transfusions prior to stem cell collection and exploring an
alternate hematopoietic stem cell procurement method with the goal
of increasing transduced cell dose. Enrollment has begun under this
modified protocol, and the DP VCN for the first patient enrolled
under the new protocol was 3.3 c/dg, with 83% of the stem cells
LVV+, with infusion planned for early 2017.
Interim data from the HGB-206 study were highlighted today in an
oral presentation by Julie Kanter, M.D., Medical University of
South Carolina, Charleston, SC.
Interim Results from a Phase 1/2 Clinical Study of
LentiGlobin™ Gene Therapy for Severe Sickle Cell Disease (Abstract
#1176)
HGB-206 is an ongoing, open-label study designed to evaluate the
safety and efficacy of LentiGlobin drug product in the treatment of
subjects with severe SCD. Results, as of November 9, 2016,
include:
- Seven patients with severe SCD have
been infused with LentiGlobin drug product under the original study
protocol. All patients are 18+ years of age with a history of
symptomatic SCD, adequate organ function/performance status and no
previous hematopoietic stem cell transplant or gene therapy.
- The median LentiGlobin drug product
cell dose was 2.1 x106 CD34+ cells/kg (range: 1.6 – 5.1 x 106
cells/kg)
- The median LentiGlobin DP VCN was 0.6
c/dg (range: 0.3 – 1.3 c/dg)
- The median VCN in peripheral blood at
last measurement was 0.09 c/dg (range: 0.05 to 0.24 c/dg)
- Patient 1309 has seen a steady increase
in hemoglobin levels and is producing 2.0 g/dL HbAT87Q with 22.8%
overall anti-sickling Hb (HbAT87Q + HbF) even after a substantial
drop in VCN between DP and peripheral blood at latest follow up
(0.9 to 0.24 at nine months follow up). As of the data cutoff, this
was the only patient in HGB-206 who received chronic transfusions
prior to receiving LentiGlobin drug product.
- At last follow up, all treated patients
were producing measureable HbAT87Q, with a range of 0.1 – 2.0 g/dL
HbAT87Q at last follow-up. Median follow up: 11.5 months (range:
8.1 – 17.1 months).
- The safety profile of LentiGlobin
treatment in severe SCD remains consistent with bone marrow harvest
and myeloablative conditioning
- Ten Grade 3 bone marrow harvest-related
AEs were reported in three patients, including one SAE
(pain/prolonged hospitalization)
- Six patients experienced at least one
SAE post-DP infusion
- No AEs reported as related to
LentiGlobin DP
Cerebral Adrenoleukodystrophy Program
Updatesbluebird bio also announced plans to expand
enrollment by up to eight additional patients in the ongoing
Starbeam Phase 2/3 clinical study of Lenti-D drug product in
patients less than 18 years of age with cerebral
adrenoleukodystrophy (CALD). The expansion of the study is intended
to enable the first manufacture of Lenti-D in Europe and subsequent
treatment of subjects in Europe, and to bolster the overall
clinical data package for potential future regulatory filings in
the United States and Europe. bluebird bio plans to begin treating
additional patients in the Starbeam study in early 2017.
Webcast Information
bluebird bio will host a live webcast at 8:30 p.m. PT (11:30
p.m. ET) today, December 5, 2016. The live webcast can be accessed
under "Calendar of Events" in the Investors and Media section of
the company's website at www.bluebirdbio.com.
About TDT
Transfusion-dependent β-thalassemia (TDT), also called
β-thalassemia major or Cooley’s anemia, is an inherited blood
disease that can cause severe anemia and can be fatal within the
first few years of life if not treated. TDT is one of the most
common genetic diseases in the world, and approximately 60,000
children are born every year with a serious form of the
disease.
Despite advances in the supportive conventional management of
the disease, which consists of frequent and lifelong blood
transfusions and iron chelation therapy, there is still a
significant unmet medical need, including the risk for significant
morbidity and early mortality. Currently, the only advanced
treatment option for transfusion-dependent β-thalassemia is
allogeneic hematopoietic stem cell transplant (HSCT). Complications
of allogeneic HSCT include a significant risk of treatment-related
mortality, graft failure, graft vs. host disease (GvHD) and
opportunistic infections, particularly in patients who undergo
non-sibling-matched allogeneic HSCT.
About SCD
Sickle cell disease (SCD) is an inherited disease caused by a
mutation in the beta-globin gene that results in sickle-shaped red
blood cells. The disease is characterized by anemia, vaso-occlusive
crisis, infections, stroke, overall poor quality of life and
sometimes, early death.
Where adequate medical care is available, common treatments for
patients with SCD largely revolve around management and prevention
of acute sickling episodes. Chronic management may include
hydroxyurea and, in certain cases, chronic transfusions. Given the
limitations of these treatments, there is no effective long-term
treatment. The only advanced treatment for SCD is allogeneic HSCT.
Complications of allogeneic HSCT include a significant risk of
treatment-related mortality, graft failure, GvHD and opportunistic
infections, particularly in patients who undergo
non-sibling-matched allogeneic HSCT.
About the Starbeam (ALD-102) Study
The Phase 2/3 Starbeam Study is assessing the efficacy and
safety of Lenti-D, an investigational gene therapy, in boys up to
17 years of age with CALD. The study involves transplantation with
a patient’s own stem cells, which are modified to contain a
functioning copy of the ABCD1 gene. This gene addition should
result in the production of functional adrenoleukodystrophy protein
(ALDP), a protein critical for the breakdown of very long chain
fatty acids (VLCFAs). Buildup of VLCFAs in the central nervous
system contributes to neurodegeneration in CALD.
Patients enrolled in the study are:
- Eligible for allogeneic hematopoietic
stem cell transplant (HSCT) but with no matched sibling donor
- Have confirmed early-stage, active CALD
as indicated by gadolinium enhancement on MRI
- Have a Loes score between 0.5 –
9.0
- Have an neurological function score
(NFS) of one or less
The primary efficacy endpoint for the Starbeam study is the
proportion of subjects who are alive and have none of six major
functional disabilities (MFDs) at 24 months post treatment. MFDs
are six symptoms captured in the Neurologic Function Score (NFS)
that, if present, are expected to severely affect the patient’s
capacity for independent living: loss of communication, cortical
blindness, tube feeding, total incontinence, wheelchair dependence,
and complete loss of voluntary movement.
About CALD
Cerebral adrenoleukodystrophy (CALD) is a rare and commonly
fatal, X-linked, genetic, neurodegenerative disease that primarily
affects young boys. CALD involves a progressive destruction of
myelin, the protective sheath of the nerve cells in the brain
that are responsible for thinking and muscle control. Symptoms
usually occur in early childhood and progress rapidly if untreated,
leading to severe loss of neurological function and eventual death
within 2-5 years in most patients. Early diagnosis is critical for
boys to receive effective treatment. The worldwide incidence rate
for ALD is approximately one in 21,000 male newborns; of those,
30-40% are affected by the cerebral form of the disease.
Currently, the only effective treatment option for patients with
CALD is allogeneic HSCT. Complications of allogeneic HSCT include a
significant risk of treatment-related mortality, graft failure,
GvHD and opportunistic infections, particularly in patients who
undergo non-sibling-matched allogeneic HSCT.
About bluebird bio, Inc.
With its lentiviral-based gene therapies, T cell immunotherapy
expertise and gene editing capabilities, bluebird bio has built an
integrated product platform with broad potential application to
severe genetic diseases and cancer. bluebird bio’s gene therapy
clinical programs include its Lenti-D™ product candidate,
currently in a Phase 2/3 study, called the Starbeam Study, for the
treatment of cerebral adrenoleukodystrophy, and its
LentiGlobin™ BB305 product candidate, currently in four
clinical studies for the treatment of transfusion-dependent
β-thalassemia and severe sickle cell disease. bluebird bio’s
oncology pipeline is built upon the company’s leadership in
lentiviral gene delivery and T cell engineering, with a focus on
developing novel T cell-based immunotherapies, including chimeric
antigen receptor (CAR T) and T cell receptor (TCR) therapies.
bluebird bio’s lead oncology program, bb2121, is an anti-BCMA CAR T
program partnered with Celgene. bb2121 is currently being
studied in a Phase 1 trial for the treatment of relapsed/refractory
multiple myeloma. bluebird bio also has discovery research programs
utilizing megaTALs/homing endonuclease gene editing technologies
with the potential for use across the company’s pipeline.
bluebird bio has operations in Cambridge,
Massachusetts; Seattle, Washington; and Paris,
France.
Forward-Looking StatementsThis release contains
“forward-looking statements” within the meaning of the Private
Securities Litigation Reform Act of 1995, including statements
regarding the Company’s research, development, manufacturing and
regulatory approval plans for its LentiGlobin product candidate to
treat transfusion-dependent ß-thalassemia and severe sickle cell
disease and its Lenti-D product candidate to treat cerebral
adrenoleukodystrophy, including statements whether the
manufacturing process changes for LentiGlobin will improve outcomes
of patients with transfusion-dependent ß-thalassemia and severe
sickle cell disease, whether the planned changes to the HGB-206
clinical trial protocol will improve outcomes in patients with
severe sickle cell disease. Any forward-looking statements are
based on management’s current expectations of future events and are
subject to a number of risks and uncertainties that could cause
actual results to differ materially and adversely from those set
forth in or implied by such forward-looking statements. These risks
and uncertainties include, but are not limited to, risks that the
preliminary positive efficacy and safety results from our prior and
ongoing clinical trials of LentiGlobin and Lenti-D will not
continue or be repeated in our ongoing, planned or expanded
clinical trials of LentiGlobin or the ongoing expanded clinical
trial of Lenti-D, the risks that the changes we have made in the
LentiGlobin manufacturing process or the HGB-206 clinical trial
protocol will not result in improved patient outcomes, risks that
the current or planned clinical trials of LentiGlobin and Lenti-D
will be insufficient to support regulatory submissions or marketing
approval in the US and EU, the risk of a delay in the enrollment of
patients in our clinical studies, and the risk that any one or more
of our product candidates will not be successfully developed,
approved or commercialized. For a discussion of other risks and
uncertainties, and other important factors, any of which could
cause our actual results to differ from those contained in the
forward-looking statements, see the section entitled “Risk Factors”
in our most recent quarterly report on Form 10-Q, as well as
discussions of potential risks, uncertainties, and other important
factors in our subsequent filings with the Securities and Exchange
Commission. All information in this press release is as of the date
of the release, and bluebird bio undertakes no duty to update this
information unless required by law.
View source
version on businesswire.com: http://www.businesswire.com/news/home/20161205006373/en/
Investors:bluebird bio, Inc.Manisha Pai,
617-245-2107mpai@bluebirdbio.comMedia:bluebird bio, Inc.Elizabeth
Pingpank, 617-914-8736epingpank@bluebirdbio.comorPure
Communications, Inc.Dan Budwick, 973-271-6085
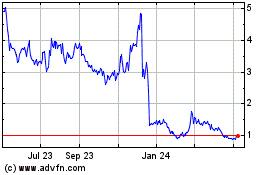
bluebird bio (NASDAQ:BLUE)
Historical Stock Chart
From Mar 2024 to Apr 2024
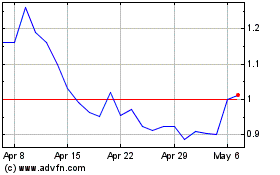
bluebird bio (NASDAQ:BLUE)
Historical Stock Chart
From Apr 2023 to Apr 2024